Provider Newsletter November 2018
 Practice Tactics
Practice Tactics
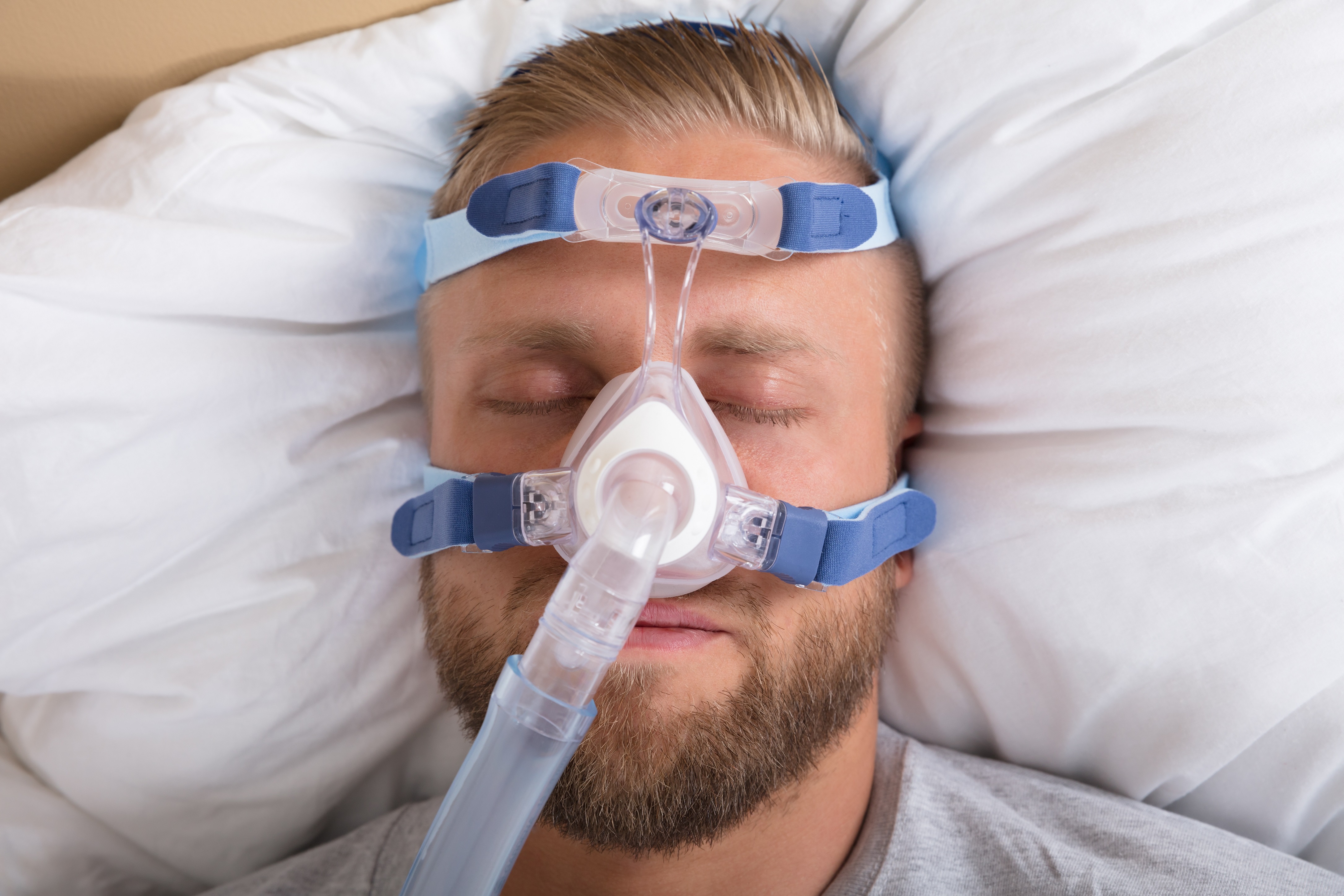
Rx after Home Sleep Study
After you have confirmed the diagnosis of Obstructive Sleep Apnea on a home sleep study, the next step is to prescribe Auto-titrating PAP for your patient. UHA authorizes a 3-month trial period for A-PAP rental. Purchase out of the machine then requires documentation of adequate utilization by the member, as provided in the SIM card download. The Rx typically includes a range of pressure that can provide the positive pressure required in various sleep positions. A typical Rx is 4 to 15 (or 20) cm H2O. The vendor should provide RT support to work with your patient to ensure the choice of mask/headgear and device settings to maximize compliance with therapy.
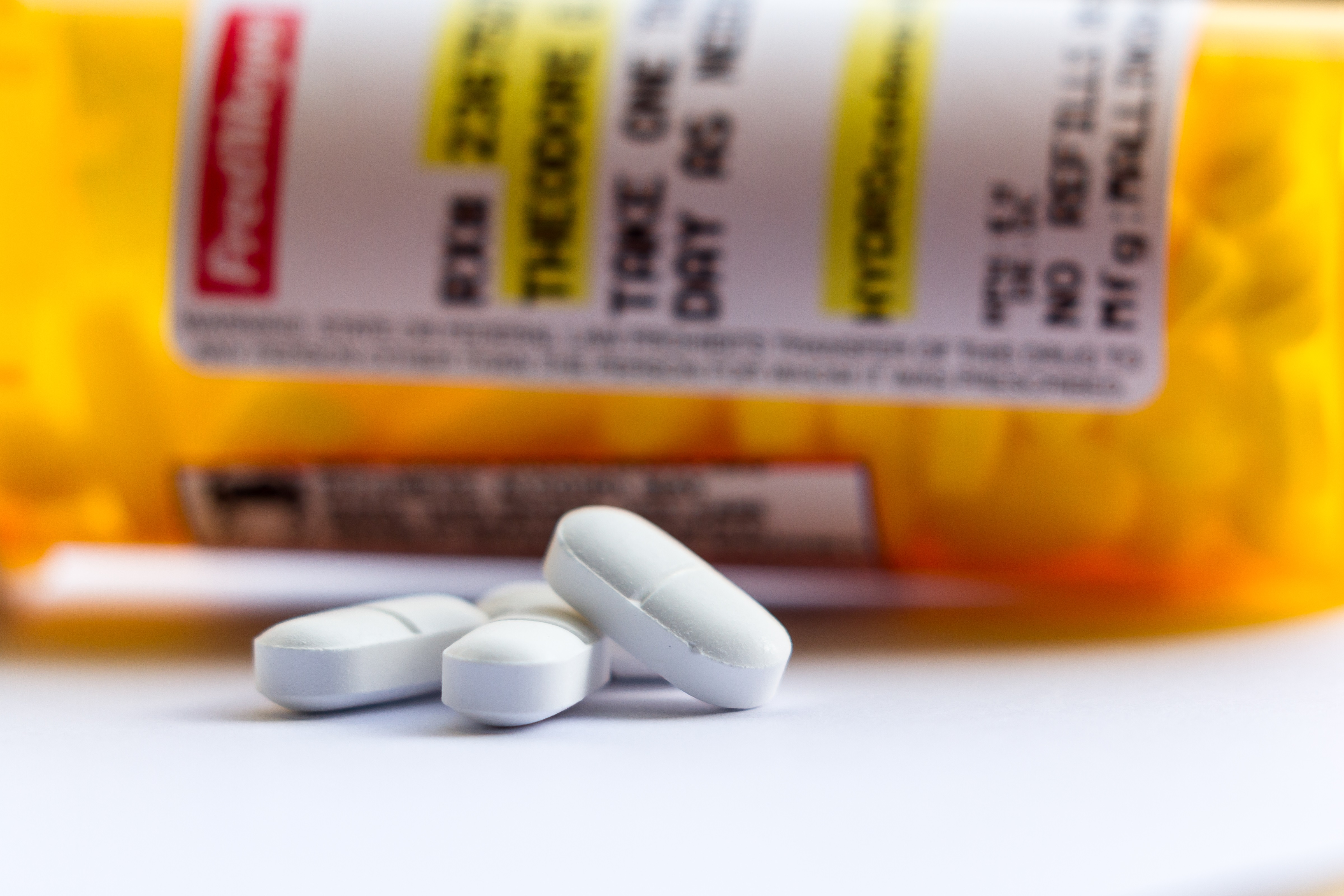
OHA Publishes Statewide Acute Opioid Prescribing Guidelines
The Oregon Health Authority recently released the Oregon Acute Opioid Prescribing Guidelines, in an effort to help clinicians working in surgical, dental, primary care, emergency and urgent care settings make evidence-based prescribing decisions when treating pain.
Opioid painkillers are powerful medications that come with risks. While they’re effective in treating acute, non-cancer pain, high doses and long-term use could lead to dependence, abuse, overdose and death. In Oregon, five people per week die of opioid-related overdoses.
The guidelines, developed in consensus with an external work group representing public health, health care and coordinated care organization leaders, build on Oregon prescribing guidelines for chronic pain, published in 2016. The acute prescribing guidelines focus on acute pain management for patients who are new to opioids. They are not intended for those who currently receive opioids nor for those with a history of substance use disorder.
Common examples of relevant clinical situations include: wisdom teeth extractions, sports injuries and post-surgical pain management. It is common practice for patients to be prescribed 30-day prescriptions in these settings. The new guidelines advise that the lowest effective dose of short-acting opioids be prescribed for no more than three days in most cases.
“While opioids are effective medications in acute pain management, many people do not use all of the pills that are prescribed by their doctors after an acute event,” said Katrina Hedberg, MD, state health officer at OHA. “What this tells us is that patients may not need as many pills as we think, and other forms of pain management may be safer and just as effective. It also tells us that there are many excess pills sitting in medicine cabinets, which could be misused or stolen.”
The guidelines could also help prevent patients with acute pain from becoming dependent on opioids long term. According to a 2017 analysis by the Centers for Disease Control and Prevention, 30 percent of those who receive an initial 30-day prescription of opioid painkillers remained on opioids a year later.
In general, the guidelines advise against using opioids as the first-line therapy for mild to moderate pain. If opioids are deemed appropriate and likely effective for the patient, the guidelines emphasize the following principles:
- Evaluate the patient.
- Assess history of long-term opioid use or substance use disorder.
- Check the Prescription Drug Monitoring Program, which tracks prescribed controlled substances such as opioids and benzodiazepines.
- Provide patient education.
- Prescribe the lowest effective dose of short-acting opioids for no more than three days in most cases and no more than seven days in cases of more severe acute pain.
- Provide follow-up and reassess pain, healing and function.
- Implement, monitor and document pain management practices to ensure care safety and quality.
The full guidelines can be found on the OHA website here.
See opportunity for pain management CME in the CME for Thee section!
 On the Lookout
On the Lookout
Antibiotic Awareness
November 13 through 19 is U.S. Antibiotic Awareness Week. During this week we remind all Oregonians to use antibiotics as prescribed and to remember that antibiotics are not effective in treating viral infections, such as the common cold or flu. The numbers of antibiotic resistant bacteria are growing, making it harder to find an antibiotic that works when we really need them. Providers can help:
- Promoting adherence to appropriate prescribing guidelines among providers. Antibiotics do not help non-streptococcal sore throats.
- Decreasing demand for antibiotics for viral upper respiratory infections among healthy adults and parents of young children. URI’s don’t get better with antibiotics but antibiotics do contribute to side effects and to antibiotic resistance.
- When antibiotics are needed, use narrow spectrum antibiotics. The drugs of choice for otitis media and strep are the penicillins and more broad spectrum antibiotics should be reserved for special circumstances.
 Medical Management
Medical Management
Antibiotics for Urinary Tract Infections in Older People
Urinary tract infections (UTI) are one of the most common infections in the older population, occurring both in the community and in long-term care settings. The spectrum of UTI ranges from symptomatic bacteriuria to bacteremic infection. UTI with bacteremia has a high mortality in the older population, with studies reporting a 28-day mortality of 5%.
Too often, the diagnosis of UTI is made in the absence of a typical clinical history or signs resulting in overdiagnosis and overtreatment. Studies suggest that UTI is incorrectly diagnosed in as many as 40% of hospitalized older people. The increasing prevalence of health care-associated infection such as Clostridium difficile and emerging antibiotic resistance highlights the importance of obtaining a firm diagnosis, treating with appropriate antibiotics and avoiding the use of broad spectrum antibiotics. There is a paucity of evidence-based guidelines for the management of UTI specifically in an older population. The aim of this Choosing Wisely Topic is to review the current evidence on the diagnosis, management, and prevention of UTI in older people.
Epidemiology
Case definitions are central to any discussion about the epidemiology of UTI. Symptomatic UTI requires the presence of new urinary tract symptoms such as frequency, urgency, dysuria, new incontinence, or costovertebral or suprapubic tenderness. The diagnosis of UTI is actually very difficult because there are no currently available diagnostic techniques for demonstrating that bacteria have invaded the tissues of the urinary tract. The diagnosis is therefore clinical and is based on symptoms or signs of inflammation of the urinary tract. Urine culture does not establish the diagnosis of UTI but does aid in the selection of appropriate treatment.
Several factors predispose older patients to UTI. Use of urinary catheters and external urine collection devices increase the frequency of bacteriuria. Asymptomatic bacteriuria is more common in patients with cognitive impairment and urinary and fecal incontinence. Neurological conditions such as cerebrovascular disease, Alzheimer’s disease, and Parkinson’s disease are all common in later life and are associated with impaired bladder emptying. Patients with diabetes mellitus also have increased prevalence of asymptomatic bacteriuria with contributing factors including neurogenic bladder and poor glycemic control. In women, postmenopausal estrogen deficiency has been linked with recurrent UTI. Cystoceles, significant postvoiding residual urine volumes, and incontinence are all associated with recurrent UTI. In men, prostatic disease leads to urinary symptoms and urinary retention. Any urological condition that can cause obstruction such as stones or tumor also increases the risk of urinary infection. Urinary tract infection most commonly arises from ascending infection via the urethra with Gram-negative organisms in the perineal region from bowel flora. Bacteriuria is defined as the presence of bacteria in urine on microscopy or quantitative culture. It is important to appreciate that the presence of bacteriuria does not always represent disease. Pyuria represents the presence of white blood cells in urine. White blood cells may be present without bacteriuria and are particularly associated with the presence of a urinary catheter, stone, tumor, or infection of the lower genital tract. Urinary tract infections are subclassified into complicated and uncomplicated UTI. Complicated UTI implies that the urinary tract has a functional or structural abnormality, but the term also includes all upper UTI and all UTI in men. Older female patients frequently have functional or structural abnormalities of the urinary tract and many regard UTI as complicated UTI in this group.
 Diagnosis
Diagnosis
Clinical findings
The diagnosis of infection in an older patient is often complicated by the lack of typical symptoms and a clear history. Up to one-third of elderly patients do not present with pyrexia in response to infection. The presence of cognitive impairment and communication difficulties can make it difficult to obtain an accurate history. Many older patients have chronic genitourinary symptoms and it is important to recognize that this is not synonymous with infection. Many clinicians incorrectly attribute factors such as functional decline, increased confusion, and nonspecific signs and symptoms to urinary tract infections and start treatment on this basis. In the absence of clear urinary tract localizing symptoms and signs, older patients should be systematically assessed with a full clinical evaluation performed to arrive at a differential diagnosis.
Urine culture
Significant bacteriuria is commonly defined as greater than 105 colony forming units/mL of a single bacterial species in a freshly voided sample of urine. Obtaining urine cultures can be difficult in some older people. Guidelines suggest that an in-and-out catheter may be the most reliable way of obtaining a urine sample in the female population if a voided sample cannot be obtained. Urine culture by needle aspiration of the bladder is the gold standard method for diagnosing bacteriuria but is rarely used in older people. Urine cultures should not be sent in individuals who are asymptomatic. Urine should also not be sent for culture based on positive urine dipsticks if no symptoms are evident.
Asymptomatic bacteriuria
Asymptomatic bacteriuria is defined as the presence of bacteria in urine on microscopy or quantitative culture in a specimen obtained from a patient who does not have typical symptoms of a urinary tract infection. This requires confirmation by two consecutive samples. Studies have suggested a prevalence rate of 25%–50% of women and 15%–40% of men without catheters amongst nursing home residents.
Risk factors associated with asymptomatic bacteriuria include institutionalization, presence of a urinary catheter, female sex, increasing age, and diabetes. It is widely recognized that asymptomatic bacteriuria should not be treated with antibiotics in the elderly population. Treating asymptomatic bacteriuria does not reduce mortality and can cause harm. Guidelines suggest that for every three people treated with antibiotics, one will come to harm. Evidence also suggests that treating asymptomatic bacteriuria in nursing home patients who have chronic stable incontinence does not improve incontinence in the short-term.
 Catheter-associated UTI
Catheter-associated UTI
Catheter-associated UTIs account for a high proportion of health care associated infection and are common among the older population in long-term care. In ambulatory patients, single catheter insertion is associated with urinary tract infection in 1%–2% of patients. Indwelling urinary catheters lead to almost universal bacteriuria within 3–4 days of catheterization. Catheterization allows for the formation of a biofilm between the catheter and urethral mucosa. A biofilm is the aggregation of microorganisms that form a structure on solid surfaces. The greatest risk factor for catheter-associated UTI is duration of catheterization.
Prevention of catheter associated UTI
Catheter associated UTI is the most common health care associated infection throughout the world and is common in long-term care facilities. Urinary catheterization should be avoided unless there is a clear clinical indication. Catheters should be avoided where possible for the management of incontinence. Staff should also be trained on indications for catheterization and written protocols should be put in place. Catheters should also be removed the moment that they are no longer required.
Alternatives to indwelling urethral catheters should be considered. Condom catheters are associated with a lower incidence of bacteriuria; however, their use is sometimes difficult in confused patients. A Cochrane review on short term urinary catheterization in adults found that suprapubic catheterization was associated with less bacteriuria than urethral catheterization. Suprapubic catheterization does carry a small risk of visceral injury on insertion through the abdominal wall. Intermittent catheterization was also associated with a lower risk of bacteriuria when compared to indwelling catheterization in this review, however studies included were mainly in an elective orthopedic setting. Guidelines suggest that antibiotic prophylaxis should not be used to prevent catheter associated UTI in catheterized patients. Although prophylaxis may decrease the incidence of asymptomatic bacteriuria in catheterized patients, it increases the risk of antimicrobial resistance.
Conclusion
Urinary tract infections present a significant problem in both hospital medicine and general practice. The burden of infection is high and there are many challenges in diagnosis and management. Several studies have identified the need for better education on asymptomatic bacteriuria and presentation of UTI in the elderly population. Symptomatic infections are often difficult to diagnose in older populations where there are high levels of cognitive impairment and communication difficulties, such as amongst residents of institutional care.
A strategy of observing patients for possible symptoms before initiating antibiotics have been advocated, although recognizing this may not always be practical in a primary care setting. Reducing inappropriate prescribing of antibiotics for asymptomatic bacteriuria is likely to reduce antimicrobial resistance. With emerging knowledge on antibiotic resistance and health care-associated infection, guidelines need to be updated to reflect the need to prescribe narrow spectrum agents when available and avoid empirical use of broad spectrum antibiotics.
Key points
- Urinary tract infections are over diagnosed and overtreated in older people.
- Diagnosis of UTI in an older person requires the presence of new urinary symptoms.
- Asymptomatic bacteriuria is very common in later life and should not be screened for or treated.
- Local guidelines and antibiotic policies should be used for management of UTI.
- Narrow spectrum antibiotics are generally preferable to broad spectrum agents.
 CME for Thee
CME for Thee
HealthInsight (Oregon’s designated Quality Improvement Organization (QIO)) is excited to announce a new opportunity to earn 6 AMA PRA Category 1 Credits™ which can also be used toward the Oregon pain management continuing education requirement. The RELIEF+ learning management system allows individuals to engage in a complimentary self-paced, high-quality training opportunity where you will learn – from national, state, and local experts – about best practices for optimal multi-faceted, compassionate pain management for older adult patients. Click here to learn more about RELIEF+.